This is a network committed to advancing clinical understanding through real-world outcomes. We believe veterinarians hold unparalleled insight into what truly works in practice. Each week, we pose one focused clinical question to the veterinary community. On Mondays, we present the question. On Fridays, we share your responses—highlighting the treatments and protocols delivering the best outcomes. Together, we’re building a living library of frontline veterinary wisdom.
Announcing: CareVet Clinical Outcomes Showcase
ALL Veterinary professionals at every level (no licensure required) are encouraged to submit solutions, ideas, innovations, or practices that are meaningfully advancing clinical outcomes – for a chance to earn $5,000.
When recommending a dental procedure in a senior pet, in your experience, what is the most common reason a pet owner may decline the procedure?
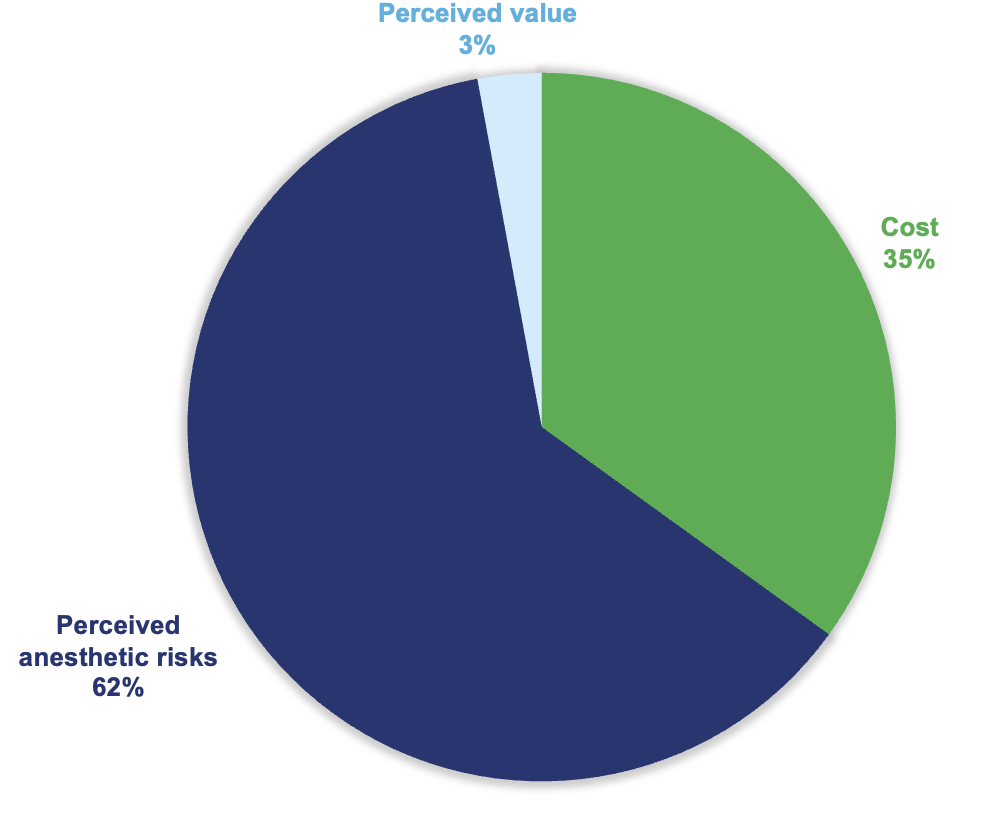
Responding DVMs were asked to identify the single most common reason a pet owner declines a recommended dental procedure in a senior patient. Responses were collected across both specialty referral and general practice settings.
Notable finding: Pet anxiety and drop-off concerns received zero selections as a primary barrier — yet responding DVMs consistently identify it as among the most emotionally charged conversations in the exam room. Its absence from survey data likely reflects that it is rarely the stated reason for decline, even when it is a significant undercurrent. Practitioners are encouraged to probe for it even when it goes unvoiced.
The dominance of anesthetic risk fear — cited by nearly two in three responding DVMs — confirms what many clinicians suspect: this is not primarily a financial problem. It is an information and trust problem, and it demands a clinical communication response, not a pricing response.
CLINICAL PERSPECTIVE
Senior Pet Dental Procedures
Why This Question Matters
Periodontal disease affects an estimated 80% of dogs and 70% of cats by age three — and by the time a patient reaches senior status, the accumulation of untreated oral pathology can be significant. Yet despite clear clinical indications, a substantial proportion of recommended dental procedures in senior pets are declined at the consultation stage, leaving animals in preventable pain and practitioners navigating a conversation that has no clean script. For veterinary professionals, this creates a persistent tension: the medical necessity is real, the evidence base is strong, and the window for intervention narrows with each visit. Understanding why owners decline — not just that they decline — is essential to closing that gap and delivering better outcomes for senior patients. Responding DVMs across small animal practices were asked to identify the primary drivers of procedure refusal in senior patients. What follows is a summary of findings, clinical context, and evidence-informed talking points for navigating these conversations.
“The decision to decline a dental procedure is almost never made carelessly. It is made by a pet owner who loves their animal and is genuinely afraid of something — our job is to find out what that something is.”
What Pet Parents Are Really Worried About
When a pet owner declines a recommended dental procedure for their senior animal, the word “no” is rarely the full story. Behind each refusal is a specific, often deeply emotional concern — and the category of that concern determines everything about how the conversation should proceed. Pet parents of senior animals carry a particular weight: they are already acutely aware of their pet’s aging, often hypervigilant about any intervention that might accelerate decline, and frequently armed with misinformation gathered from online forums, social media, and well-meaning friends. Fear of anesthesia in particular has taken on a life of its own in the pet-owning community, fed by anecdote and outdated assumptions that do not reflect modern perioperative care standards. Cost concerns, while real, are often entangled with value questions — an owner who says “I can’t afford it” may also be asking, implicitly, “is this truly worth it for a dog her age?” Recognizing the difference between a financial barrier and a perceived-value barrier is a critical skill in the exam room.
How to Navigate These Conversations with Clients
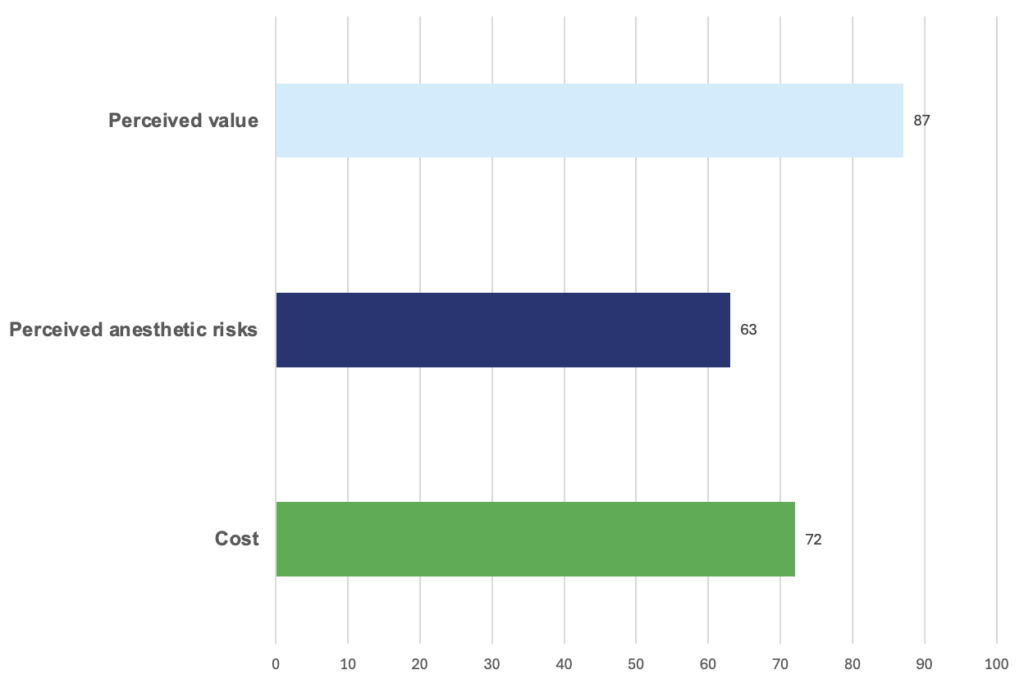
The following talking points are drawn from responding DVM feedback and evidence-based communication
frameworks. They are intended as anchors for a productive conversation — not scripts — and should be adapted to your practice voice and the individual owner.
Perceived anesthetic risk: PRIMARY BARRIER
Key messages to communicate:
• Lead with data, not reassurance. Vague comfort (“don’t worry”) feels dismissive; sharing pre-anesthetic bloodwork results and an ASA physical status classification invites the owner into the risk assessment process.
• Contextualize the statistics. Modern perioperative mortality rates for ASA I–II patients are low — share the numbers directly. The Brodbelt et al. (2008) data remains a useful reference for real-world anesthetic risk in small animals.
• Address “too old for anesthesia” directly. Age alone is not an anesthetic contraindication. Pre-procedure screening — bloodwork, blood pressure, cardiac assessment — determines risk, not the number on the chart.
• Clearly distinguish from anesthesia-free dentistry. Per the AVDC position statement, procedures without general anesthesia cannot provide the same diagnostic or therapeutic benefit and carry their own risks. This is a patient safety issue.
• Walk through the monitoring protocol. Describing IV catheter placement, fluid support, continuous monitoring, and a dedicated anesthesia team helps owners visualize the safety net around their pet.
Phrases that tend to land well;
“We run bloodwork first specifically so we know what we’re working with — nothing goes forward until we’ve reviewed those results together.”
“The risk of anesthesia for a patient in good baseline health is quite low. The risk of leaving this untreated is not.”
Cost: SECONDARY BARRIER
Key messages to communicate:
• Reframe cost as a comparison, not an absolute. The upfront cost of a dental procedure competes with an invisible future cost — emergency extractions, chronic pain management, repeated antibiotics, and potential systemic complications.
• Quantify the cost of inaction. Where possible, give a realistic estimate of what management-without-treatment might cost over 12–24 months. Specific numbers are more persuasive than general statements.
• Offer practical pathways. Payment plans, pet insurance reimbursement, and staged treatment can transform a declined procedure into a scheduled one.
• Acknowledge the concern without minimizing it. “I understand this is a significant investment” opens the conversation; dismissing financial hesitation closes it.
Phrases that tend to land well:
“The cleaning we’re recommending today is almost always less expensive than the treatment we’ll be looking at in 12 months if we wait.”
“We can talk through options for how to approach this financially — there are a few paths that might work for your situation.”
Perceived value: RARELY CITED
Key messages to communicate:
• Make pain visible. Dogs and cats are stoic — owners frequently don’t know their pet is in pain. Describing the clinical signs of oral discomfort (reluctance to chew, behavior changes, weight shifts) helps owners recognize what they may have attributed to “getting older.”
• Connect oral health to systemic health. Untreated periodontal disease has documented associations with cardiac, renal, and hepatic pathology. Framing dental care as whole-body preventive medicine — not a cosmetic service —resets the value equation.
• Use quality-of-life language. “Comfortable senior years” is a goal almost every owner shares. Dental care is a direct pathway to that outcome.
• Before-and-after case examples are powerful. A brief description of a patient who resumed normal eating or play after a dental procedure is often more persuasive than any statistic.
Phrases that tend to land well:
“One of the things we can’t easily see is how much discomfort she may be quietly managing. Dental disease is one of the most common hidden sources of pain in senior dogs and cats.”
“We had a patient similar to yours last year — after the procedure, the owner said it was like having a two-year-old dog back.”
Pet anxiety & drop-off concerns: UNDERREPORTED
Key messages to communicate;
• Probe for this concern even when it isn’t stated. Survey data shows zero responding DVMs selected drop-off anxiety as the primary reason for decline — which suggests it often operates beneath the surface, disguised as another objection.
• Offer a pre-visit pharmaceutical protocol proactively. Trazodone or gabapentin administered the night before and morning of the procedure can meaningfully reduce procedural stress for the patient and owner hesitation.
• Eliminate the unknown. Walk owners through what their pet’s day actually looks like: who greets them at drop-off, where they rest, how monitoring is conducted, when the owner will receive updates.
• Acknowledge the emotional component for the owner. Senior pet owners are often processing anticipatory grief. A moment of recognition — “I know it’s hard to leave her” — builds trust before any clinical argument is made.
Phrases that tend to land well:
“We can send you a medication to give him the night before so he arrives relaxed. Most owners tell us it makes a real difference — for the dog and for themselves.”
“We’ll text you when she’s under, when she’s waking up, and when she’s ready. You won’t be in the dark.”
References
-
1. Bellows J, Berg ML, Dennis S, et al. 2019 AAHA Dental Care Guidelines for Dogs and Cats. J Am Anim Hosp Assoc. 2019;55(2):49–69.doi:10.5326/JAAHA-MS-6933
2. Brodbelt DC, Blissitt KJ, Hammond RA, et al. The risk of death: the confidential enquiry into perioperative small animal fatalities. Vet Anaesth Analg. 2008;35(5):365–373. doi:10.1111/j.1467-2995.2008.00397.x
3. Niemiec BA. Periodontal disease. Top Companion Anim Med. 2008;23(2):72–80. doi:10.1053/j.tcam.2008.02.003
4. Clarke DE, Kelman M, Perkins N. Effectiveness of a vegetable dental chew on periodontal disease parameters in toy breed dogs. J Vet Dent. 2011;28(4):230–235.
5. Watkins K, Wiese AJ. Anesthetic risk stratification in the geriatric small animal patient: clinical considerations and communication frameworks. Vet Clin North Am Small Anim Pract. 2022;52(3):561–578.
6. American Veterinary Dental College (AVDC). Position Statement on Anesthesia-Free Dentistry. Published 2013; revised 2020. Accessed 2024. https://avdc.org/avdc-nomenclature/
7. Veterinary Oral Health Council (VOHC). Accepted Products for Dogs and Cats. http://www.vohc.org. Accessed 2024.
8. Döring S, Rosenberg M, Saran J, Scholz A. Client communication strategies to improve uptake of recommended dental procedures: a retrospective practice audit. J Am Vet Med Assoc. 2023;261(7):987–993.
Clinical Outcomes Annual Report
This report brings together the answers to more than fifteen of this year’s most important clinical questions, offering a comprehensive view of what is working in practices across the country.
Subscribe today and become part of the Clinical Outcomes Network.
Check Out Past Results
See how veterinarians nationwide answered previous Clinical Outcomes questions and what their results reveal.



2 Comments. Leave new
Love the result/pie chart!
Excellent resource